The Diagnostic Odyssey – A Mother’s Experience
The diagnostic odyssey is a term used to describe the long and arduous journey that many rare disease patients find themselves on in pursuit of a diagnosis. The charity, Rare Disease UK, estimate that a patient with a rare disease will wait an average of four years for a diagnosis and be given an average of three misdiagnoses. This not only impacts the patient’s clinical outcomes from the rare disease but also their mental health, work/school life and the whole family. Rare Disease UK published the ‘Rare Reality’ report this year which gives an insight into the patient and family experience of living with a rare disease. This is really important work, enabling doctors to understand the lived experience of those with rare diseases and their families.
In this article Sarah describes her family’s diagnostic odyssey as they struggled to find a diagnosis for her daughter, Millie. Sarah first suspected that all was not right with Millie when she was a newborn baby however it was a number of years before they received an accurate diagnosis. Millie, now 4 years old, was eventually diagnosed with congenital sucrase-isomaltase deficiency (CSID).
When did you first know something was wrong with Millie?
We first knew that all was not quite right with Millie when she was two weeks old. She would scream in pain relentlessly for hours at a time, writhing in my arms. She would have terrible diarrhoea and vomited constantly, making it very difficult for us to leave the house.
You have an older daughter – was your experience with Millie very different?
Millie has an older sister Mia and two older half sisters, so we knew that something definitely wasn’t right – Mia had had a few issues with ‘reflux’ but nothing compared to this.
When was the first time you sought help from the medical profession?
After holding a screaming 1month old baby for hours on end my husband would have to come home from work to take over and we’d end up heading to A&E as we were at a loss to know how to help her. We’d tried some over the counter remedies to ease her but nothing seemed to work or it even made her worse. We were then referred into the hospital paediatric department with an open admission to the ward.
Millie was misdiagnosed many times – can you name some of those misdiagnoses?
Millie was at first treated for reflux and silent reflux. We were prescribed hefty medicine for this and discharged. We were then told she must have CMPA (Cows Milk Protein Allergy). We removed dairy from my diet. We were told to wean her at 4 months, and couldn’t find any formula milk she could take. She vomited everything. She was then therefore diagnosed as F-PIES (Food Protein Induced Enterocolitis Syndrome). Then gut motility issues. Then SIBO (Small Intestine Bacterial Overgrowth). Then irritable bowel syndrome.
Given the symptoms of abdominal pain, difficulty feeding and vomiting – a cow’s milk protein allergy seems like a fair differential diagnosis; however Millie showed no improvement on the extensively hydrolysed formulas. Did anyone ever suggest a different kind of intolerance or enzyme deficiency? And at what point do you think the team should have considered a different diagnosis?
We were under the care of the paediatric allergy team and they conducted blood tests for IgE allergies, but nothing conclusive was discovered. At no point did anyone suggest she might have an enzyme deficiency. We felt as though the team were not convinced that there was much wrong with Millie as she continued to follow a healthy weight line. It was even suggested that the problem might be in my head. As we tried to wean Millie onto food the problem became worse as everything we tried seemed to make her vomit, and she had constant diarrhoea. We found she could tolerate Nanny Care Goats Milk and she drank a lot of it, which is why her weight was ok for a while. It was only when her weight plateaued for ten months that they began to take us seriously. At this point we were referred to the gastroenterology team where we asked them to check Millie for coeliac disease and CSID as we had realised she could not tolerate any form of sugar.
I know you had some very difficult consultations. Are there any that standout in your mind and what made them difficult?
The worse consultation we had was with the first consultant. She had Millie’s blood test results in front of her and she said they were all completely normal, but we could see that more than half were highlighted as abnormal. We asked her to rule out CSID specifically. She said that to do that we would have to make Millie poorly for a minimum of 8 weeks for the tests to show anything. We knew that was not the case. She also said that she wanted to leave it for a year until Millie could speak and tell us herself how she felt. Millie was 2 at the time and only able to eat 5 foods and we were feeling desperate. I said this and the consultant immediately asked if she could write to my doctor as I clearly needed help. This consultation left us feeling very cross and sad that the system seemed to be letting us down and not listening to us properly. We felt that she lacked sufficient experience to help us and we would have preferred her to acknowledge that and to try to find someone who could help us.
Millie was eventually admitted to hospital for observation. This must have presented a dilemma for you – you knew that they would give Millie foods that would cause her pain in order for them to observe her symptoms first hand. What were those couple of days on the ward like for you?
The time we spent on the ward were probably the worst 48 hours of our journey with Millie. We had to make her poorly by giving her food that we knew she couldn’t tolerate so that the team could observe her and carry out some tests. She became so poorly so rapidly that we were sent home early. She became progressively lethargic, pale and refused to eat anything further, her stomach was very badly bloated, she had terrible diarrhoea and burns on her bottom. They were unable to carry out the tests they needed too as she refused to swallow the barium liquid and screamed. It did however seem to give the green light for Millie to have the gastroscopy and biopsies that we really wanted and this was booked in quickly after our admission.
In the end you looked for answers with homeopathy – why did you do this and how did the homeopath help?
We were so frustrated by the lack of progress with the hospital team that we decided to seek help from a renowned homeopath. We were given a tiny sucrose pill which carried the homeopathic treatment. Millie took this pill for a couple of days and seemed calmer and more relaxed, then she started vomiting violently every time we gave her the little pill. This was how we discovered that she couldn’t tolerate sucrose.
You suggested CSID as a diagnosis after the sucrose pills from the homeopath caused extreme vomiting. Do you know why this was ruled out by Millie’s team?
The gastro team said it was not possible for Millie to have CSID because it was so rare. They also admitted that they were not familiar with the condition. They referred us to a different hospital to see a different gastroenterologist.
In your blog you talk about the relief after Millie’s normal gastroscopy. However, even though her anatomy was normal, she was still unwell. What did you do next?
When we were told Millie’s gastroscopy results were normal, we were obviously relieved. However I asked to see the results as I was also surprised as I was pretty convinced by this stage that CSID was the answer. I looked at the results and realised that although the numbers were within the normal range, they were right at the lowest end of the normal range. They had also only tested for 2 of the enzymes for CSID when they should have tested for four, so we would never have had a proper diagnosis with these results anyway. We decided to seek a second opinion.
You requested a trial of Invertase from this same team. What is this drug and what happened?
In view of the fact that only two of the enzymes had been tested for and that they were very low, and that we had then put Millie on an elimination diet to eliminate starch and sugar and she had responded extremely well to this with a marked improvement in her energy levels and bowel movements, we asked for a trial of Invertase. Invertase is an enzyme replacement treatment, it is essentially a food grade yeast (similar to Sucraid in the US) which replaces the missing enzyme in the bowel and helps the body to digest sucrose. In the US a successful trial of this is considered to be an appropriate diagnostic method for CSID. The team refused the trial of Invertase as they said they had insufficient evidence that Millie had CSID.
You talk much more positively about the consultation with the CSID specialist. What was the main difference between this consultation and all the others?
Our second opinion was with a very professional and knowledgeable Professor in paediatric gastroenterology. We specifically chose him as we knew he had experience of diagnosing CSID. We immediately felt at ease with him. Unlike the other consultations, he made a thorough examination of Millie, he asked us a lot of questions and really listened to us. For the first time, he asked a lot about our family history. On reflection we found it strange that no-one had asked us much before about this as CSID is a genetic condition. If they had, they would have learned that I have never been able to tolerate sugar very well. As this was my normal, I had never questioned this or made the connection. He looked at Millie’s gastroscopy results and agreed that those, along with her very typical CSID symptoms indicated to him that she most likely had CSID. He immediately arranged for her to be put on a trial of Invertase.
When Millie was finally given invertase what changed?
The change in Millie was astonishing. Immediately she had more energy, we finally saw a cheeky little girl emerge from her years of debilitating pain and fatigue. She was more confident to try different foods. She had her first completely normal bowel movement. Everyone noticed how different she suddenly was. She smiled a lot. She ran around. She was a typical 3 year old!!
What was Millie’s diagnosis? What was it like to finally have an answer?
Millie had her second gastroscopy under the new consultant pretty quickly. He tested for all the enzymes and the results were again just within the normal range, but very low. Based on this, even though the clinical evidence from the laboratory suggested she did not have it, he diagnosed her with CSID and anaemia based on her symptoms, the huge success of the trial of Invertase, plus the success of the starch and sucrose elimination diet. We believe that instead of being rigidly beholden to ‘normal ranges’, he made a successful and appropriate diagnosis because he interpreted the lab results in conjunction with the other evidence. We now know from other CSID families that the only difference between Millie and children with lower enzyme levels is the length of time it takes for her ‘quota’ to be reached. Her symptoms once reached are just as, if not more, severe. We were very relieved to finally have a diagnosis, but at the same time sad that this would be a condition for life, that she will never grow out of and everything that brings with it.
Is Millie still receiving invertase? And where are you now in the journey?
Millie has now been permanently receiving Invertase since November, and she is now just like a normal little 4 year old girl. She takes the Invertase with every meal and snack and is still on a limited diet so that her gut has time to heal. Her bowel movements are now completely normal and she is now able to go to the loo by herself (important step for a young child!). She is full of life and energy and no longer has to rest on the sofa in the afternoons because she is too tired to walk. We are now able to test her intolerance as we can push her limits and gauge the reaction. We know she can only tolerate 8g of starch per day and less than 2g of sugar. 8 g of starch is approximately ¼ of a small potato or 10 pieces of popcorn. 2g of sugar allows her to eat a small amount of naturally occurring sugar per day such as a few green beans and 3 small florets of broccoli per day. We hope that in time she may be able to tolerate more starch.
Finally, what advice can you give to medical students and doctors that might help them diagnose a rare disease in the future?
The biggest piece of advice I would give is to take the time to really listen to the parents and to ask as many probing questions as possible. It is generally not the most pleasant thing to do to have to bring your child into hospital, the majority of parents would only do that if there really was a very good reason to do so. I would also like to think that if a doctor really does not know the answer, and does not have sufficient knowledge or experience to make a diagnosis, it is perfectly acceptable to say that and to try to find someone who can help. We don’t expect doctors to be superhuman and know everything, but we do expect someone to put their hand up and say if they don’t know enough about a particular condition. Our own GP has been excellent in this respect and has tried so hard to help point us in the right directions whilst saying she really doesn’t know anything about the condition.
A mother’s top tips for helping to improve the diagnostic odyssey:
- Listen to the parents and ask probing questions.
- Take the parents seriously – it is hard enough having a poorly child, without having your integrity questioned.
- Ask open ended questions specifically about family history – many rare diseases are genetic and there may be important clues.
- Consider that there may be more than one co-occurring diagnosis.
- Find and collaborate with someone who is more familiar with the condition being investigate.
- Do some research and ensure the correct ‘gold standard’ path to diagnosis is followed.
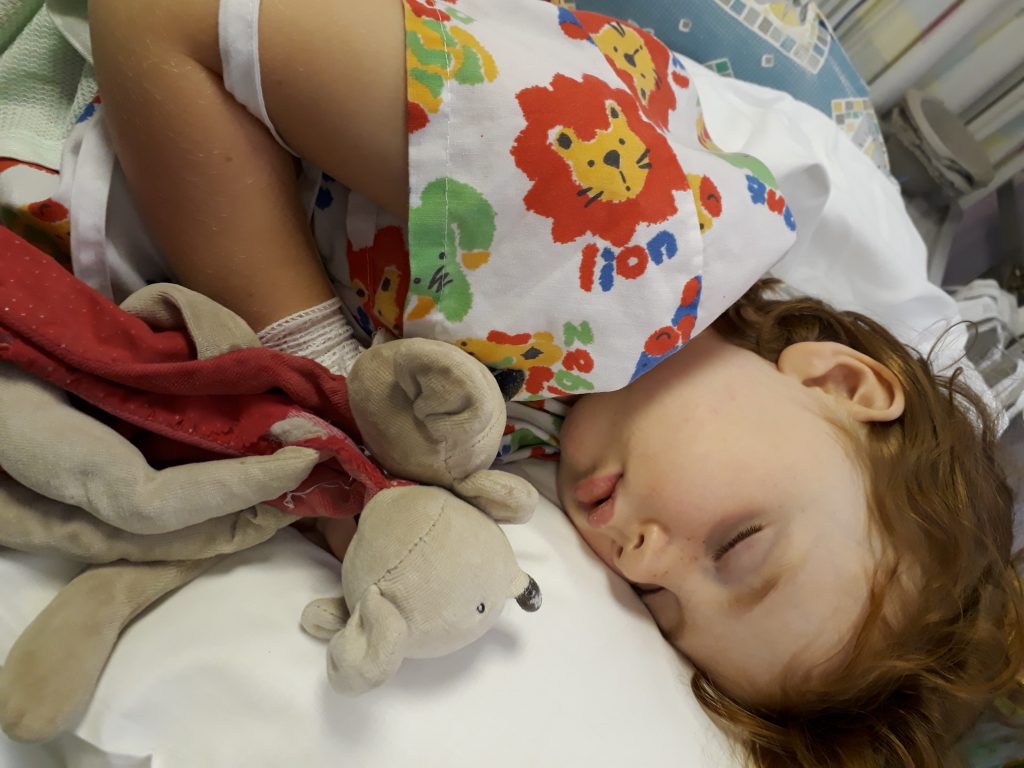
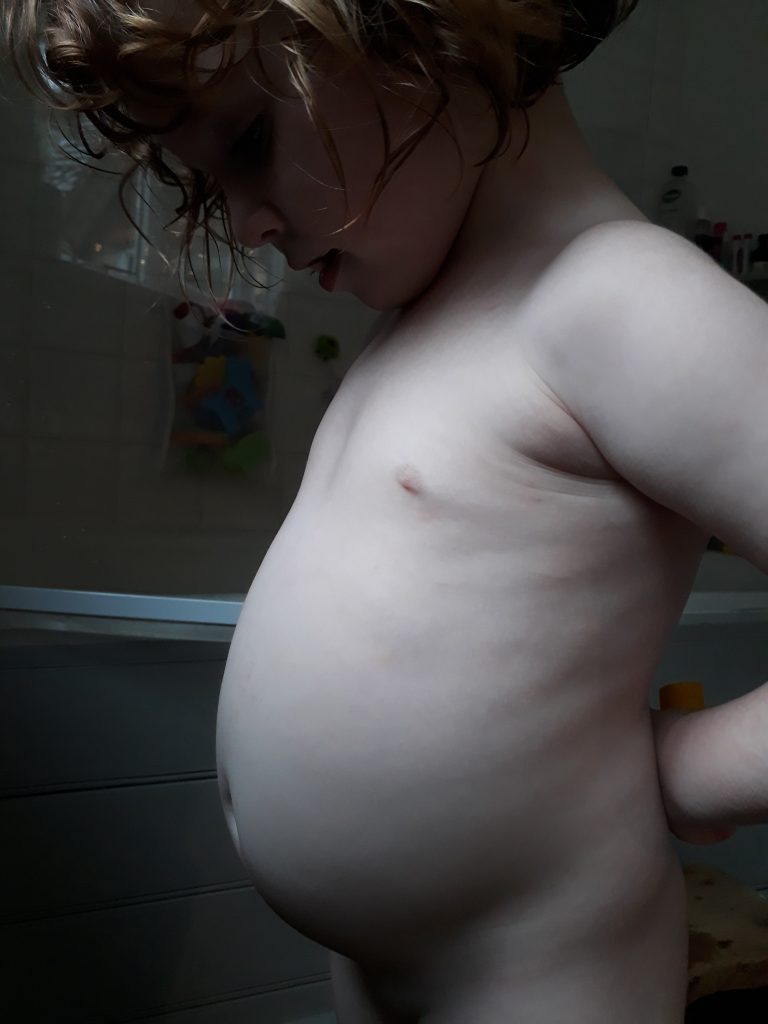
Thank you to Sarah for sharing her family’s story with us and for giving us permission to share pictures of her lovely daughter, Millie.







4th June 2019 @ 7:44 pm
Thank you Sarah and Jo for highlighting CSID and the difficult journeys family have to endure to reach a diagnosis.
Our family story was similar, diagnosis for my daughter at the age 9, many years ago.
It made me really sad to hear what you had gone though and reminded me of all the challenges and struggles we had faced, along with many others.
So pleased to read that you had treatment for Millie and hope she continues to thrive, I hope that sharing your story will help to make a difference, for patients and families of rare diseases.
2nd July 2019 @ 1:20 pm
Dear Bridgit
Thank you for your kind message of support for Sarah. I am pleased that M4RD is not only raising awareness about rare diseases but is also able to connect people so they can share experiences. I hope you will continue to follow our work.
Best wishes,
Lucy McKay – CEO of M4RD
30th September 2019 @ 10:37 pm
Dear Bridgit
Thank you so much for your kind words, sharing this difficult experience has helped a number of other families already who have reached out for support to us whilst they are experiencing a similar diagnostic odyssey. It is comforting to know that we may be able to help others in a similar situation, where the knowledge of this condition in the UK is still at a basic level.
We hope to continue to help others and Millie continues to go from strength to strength! She has just started school and the confident, bubbly little girl that skips into class every day is a world apart from the recoiled, introverted child who lived with pain and discomfort every day of her life until she turned 4.
I hope your daughter also is thriving!